|
Both Marisa de Toledo, (purple and black belted dress, left), and Steven Pete (right), have never experienced pain, and have been this way since birth.
She felt no pain during childbirth, and was comfortable enough to sleep through the experience (BBC iPlayer Radio 2015). This woman, Marisa de Toledo, has a case of what some define as congenital analgesia, or synonymously, congenital insensitivity to pain. Congenital analgesia is a defect that must be present from birth until death, rather than acquired from another disease or a traumatic injury; sufferers must have pain insensitivity occurring evenly throughout their body, and have no general physical or mental retardation (Sternbach 1963:253). Other modern cases, individuals including Steven Pete and Marisa, identify themselves as suffers of the disease (BBC iPlayer Radio 2015), and yet research dictates, “there is no case which appears to be a genuine instance of congenital insensitivity to pain” (Sternbach 1963:254). This blog post will explicitly describe how physically dangerous congenital analgesia is, to what degree it effects personality and social interaction, as well as how Marisa and Steven define their confidence in medical etiology and treatment of congenital insensitivity to pain.
The hazard of feeling no pain: each injury is amplified by lack of a signal to escape damage.
hazards of congenital analgesia, as the individual lacks both a conscious and an autonomic signal notifying them to seek help. The absence of pain with the magnifying effect of absent reflexes results in extensive physical injury that has been well documented by researchers, physicians, authority figures and those with personal experience. In alignment with the clinical description, Marisa and Steven certainly experience dangerous accidental injury due to congenital analgesia (BBC iPlayer Radio 2015). Steven’s family discovered his disease when, teething, he chewed off a quarter of his tongue (Pete 2010:1). Marisa’s doctor formally diagnosed her when she broke her ankle and could calmly walk on it, worsening the inflammation (BBC iPlayer Radio 2015). Both biomedical research and patient narrative describe the necessity of constantly being aware of physical dangers, however research focusses on the individual as the one affected, while individuals with congenital analgesia focus on not only themselves but the impact they have on their families (Genetics Home Reference 2015). Marisa and Steven rely on family; Marisa’s husband has helped lessen the severity of her accidental burns (BBC iPlayer Radio 2015) while Steven notes, “the last time I had a broken bone, my wife actually noticed before I did” (BBC News Magazine 2012:1). While both those with the condition and medical professionals agree that potential physical injury is much higher in those with congenital analgesia, they diverge when describing the number of people influenced in the sickness experience.
Social effects of congenital analgesia do not necessarily render an individual into a superhuman.
Researchers are hunting for a complete explanation of causation for the future, while those with congenital analgesia look for coping mechanisms to increase their quality of life in the present.
patients. According to Sternbach, he did not find a case of true congenital analgesia, just similar but incomplete insensitivities to pain (1963:256). However, other narratives of scientific authorities demonstrate their conviction about the success of biomedicine through ongoing research, as some studies have recently discovered that congenital insensitivity to pain may be linked to the SN9A gene; however, this finding has no direct segue into therapy or treatment (Genetics Home Reference 2015:1). Biomedical methods are determined to define a specific etiology of disease before developing therapy, and this fosters doubt about biomedicine in those who identify as having congenital analgesia, who seek treatments alongside knowledge of causation. Marisa’s mother was skeptic; she did not take Marisa to the doctor for an unfelt back injury, and Marisa herself says that “she still doesn’t understand anything about this condition” despite having visited multiple doctors (BBC iPlayer Radio 2015:1). The two narratives, in relation to their faith in biomedicine, can be also be contrasted by amount of value placed in fostering emotional wealth or research prestige. Emotional wealth, the having of essential relationships, interconnections and social belonging, is highly valued in patient narratives, but those creating clinical definitions prize exact etiology and accompanying publication recognition. Steven exemplifies how important emotional capital is to patients as he, with help, made a website to facilitate its growth through meetings of those afflicted, as “they wanted to connect with others throughout the world who we share this condition with” (Pete 2010:1). Finally, emotional wealth through upbeat outlook and empathy is seen in the patients’ effort to maintain dynamic, healthy narratives. This is indicated in the dialogue between Steven, “try to be as positive in life as you can” and Marisa, “you have to stay positive don’t you… that’s the truth.” (BBC iPlayer Radio 2015:1) Ultimately, scientific research provides eventual progress, using biomedicine, toward an etiology for congenital analgesia while patient narratives exemplify adaptive strategies for building a healthy worldview and immediate therapies that support each other socially.
In summary: Marisa and Steven highlight that key differences exist between their descriptions of congenital analgesia and the descriptions provided by social/medical authorities.
The clinical, research and biomedical authority descriptions of congenital analgesia diverge significantly from patient illness narratives. Both agree that physical dangers are compounded by insensitivity to pain, yet they are dissimilar in their identification of how many individuals are ultimately effected. Marisa and Steven's accounts do not concur with scientific conclusions about personality and social interaction; while clinical observations deem both normal, those effected highlight that social suffering can occur in the absence of physical pain. Finally, in terms of the efficacy of biomedicine and strict etiological research, clinical perspectives place faith on the anatomical search for a cause, while patients define their therapy by utilizing their emotional wealth and coping mechanisms. In summary, the overarching conclusion is that suffering in the absence of pain is underappreciated, and as difficult to treat as it is prevalent in those with congenital analgesia. As Steven clarifies, doctors understand the disease; “they just don't understand the human component of it - the psychology of what can happen when you grow up not being able to experience pain” (BBC News Magazine 2012:1).
0 Comments
Leave a Reply. |
Categories
All
Blog TeamHannah, VP Admin Archives
January 2022
|
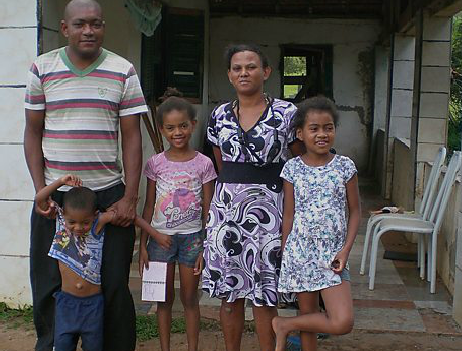




 RSS Feed
RSS Feed
